How we understand men's health
How we understand men's healthHealth outcomes are shaped by wider determinants of health (Figure 1): the social norms that we inherit, the socioeconomic conditions we live in, the relationships and expectations that surround us and the cultural norms that shape communities over generations. These factors interact with the local infrastructure, service accessibility, influencing what kinds of help they seek, what kind of actions they take and what sort of opportunities and futures feel visible and possible.
Gendered expectations describe the societal norms and stereotypes around how individuals should act, present and behave based on their sex. Commonly cited and investigated domains on gendered stereotypes include personality traits, role behaviours, occupational and emotional.
Frequently, men’s health is described through a language of personal actions or failing of action; men ‘don’t talk’ or ‘won’t seek help’ or are ‘risk takers’. Similarly to expressions such as ‘man-up’ or ‘grow some balls’, the language used to describe masculine health seems to assume that poor health is driven by personal failings and individual actions. While individual actions matter, this framing does not sufficiently recognise the influence of the social norms of what it means, or does not mean, to be a man, and how this shapes our communities and individuals. In Cumberland, these norms are shaped by a history of industrial work, de-industrialisation, tight-knit communities and a longstanding local culture towards stoicism and emotional self-reliance.
This chapter provides the conceptual grounding for understand the patterns of men’s health outcomes seen across Cumberland. It aims to situate male health inequalities in sociological context, to explore how masculinities develop and result in differential health outcomes.

Figure 1: The building blocks to health by the Health Foundation
How men's, women's and children's health interconnect
The phrase ‘health is not a zero-sum game’ is often used in relation to health. This phrase addresses the concept that one person’s health gain is another person’s health loss. ‘Positive sum’, are health investments that have wider impacts beyond the primary aim, such as improved physical health leading to improved economic productivity or social connection, simultaneously benefiting others in immediate and wider circles.
Men and women’s health are interdependent. Individual, partnership, societal and systemic interactions between genders influence physical, mental and social health.
Poor male health, whether through chronic illness, addiction, or mental ill-health, has consequences for women and children. Women may carry increased caring responsibilities, face financial strain, or encounter emotional and physical risks within relationships. Children exposed to instability, conflict or trauma may have poorer health and emotional wellbeing outcomes, which in turn can shape the outcomes of the next generation of men.
Parental wellbeing directly affects children’s emotional security, educational attainment and health development, influencing how children grow and behave. Household stressors such as poverty, grief, insecure work and poor-quality housing are experienced collectively.
From a sociological perspective, gender operates as a social system: a set of rules, expectations and practices that shape how people behave and how society responds to them. We adopt a gender-relational lens: the health of one group cannot be understood or improved without analysing gender differences, dynamics and social norms, allowing us to identify systematic drivers and design targeted solutions.
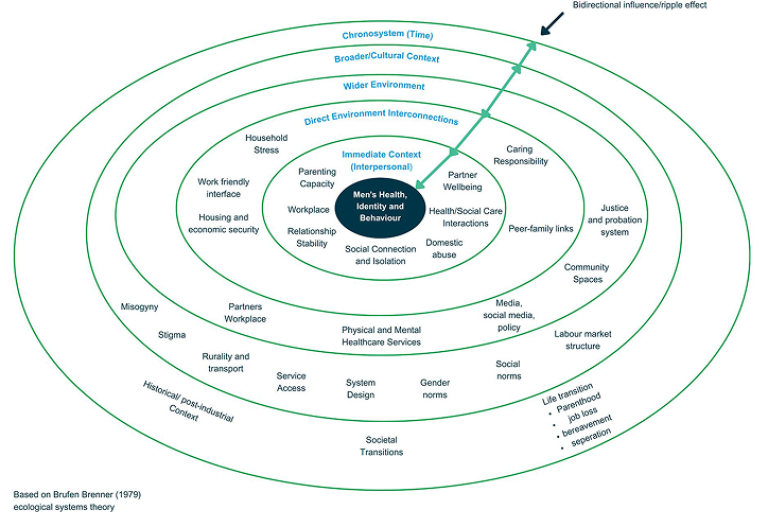
Figure 2: The bi-directional interactions between men’s health and identity, and relationships, environment and cultural. Adapted) ecological systems theory (Bronfenbrenner, 1979).
Masculinities - "being a man"
Masculinities - "being a man"Masculinity is a socially constructed set of behaviours, traits, roles, and practices associated with men and boys, which are learned and practiced through life. Most men do not consciously choose to learn these norms; they are inherited from families, peers, communities, media and workplaces.
Because masculinity is learned rather than inherent, it exists in multiple forms. These forms are shaped by social position, including class, ethnicity, age, sexuality, body and ability. Importantly, different expressions of masculinity are associated with different health risks, behaviours and outcomes, and can vary between cultures and evolve over time.
Sociologist Raewyn Connell’s framework helps to explain the social construct of ‘ideal’ masculinity in relation to femininity and other forms of masculinity. It explains patterns through which different individuals relate differently to masculinity, and how this shapes exposure to risk, vulnerability and health outcomes.
Raewyn's Connell masculinities framework
Summary of Raewyn's Connell masculinities framework and how they may shape harmful health and relationship outcomes.
Hegemonic masculinity
Definition
The culturally dominant ideal of manhood, which is typically characterised by strength, emotional control, self-reliance, heterosexuality and authority. This form establishes social expectations against which other men are measured and reinforces men's power over women and other men.
Potential health impacts for men
- reluctance to seek help or disclose distress
- late presentation to health services
- risk-taking behaviours, including substance use and dangerous driving
- emotional suppression, which increases risk of depression, suicide and relationship breakdown
Potential impacts for women and children
- reinforces unequal power dynamics in relationships, increasing women’s exposure to emotional labour, caregiving burdens, and, in some cases, coercive control or violence
- limits children’s exposure to emotional modelling, communication and helpseeking behaviours. Provides harmful role modelling for children regarding how men should act and relationship’s function
- contributes to cultures in which women’s safety concerns or emotional needs may be minimised or dismissed
Complicit masculinity
Definition
Describes men who do not fully meet hegemonic ideals but still benefit from the wider system of male privilege. These men may not actively promote dominant norms, but neither do they challenge them.
Potential health impacts for men
- adopting silence or emotional distance as a default coping strategy
- accepting harmful norms around drinking, work or stress as “just how things are”
- benefiting from male privilege in some settings while remaining vulnerable to poor health outcomes
Potential impacts for women and children
- increased strain within families as women act as mediators or carers
- reinforces silence around men's distress, delaying support and increasing the likelihood of crises that affect whole households
Subordinated masculinities
Definition
Masculinities that are devalued or stigmatised in relation to the dominant ideal, including gay men, emotionally expressive men, or those who challenge gender norms.
Potential health impacts for men
- higher exposure to stigma, discrimination and harassment
- increased rates of anxiety, depression and self-harm
- barriers to accessing safe and affirming services
- heightened social isolation
Potential impacts for women and children
- stress and marginalisation can affect relationships
Marginalised masculinities
Definition
Refers to men whose intersecting social positions, shaped by class, ethnicity, disability, care experience or poverty, limits access to power, status and resources. These men may be expected to meet dominant masculine ideals but lack the material conditions to do so.
Potential health impacts for men
- chronic stress linked to economic insecurity
- higher exposure to trauma, bereavement and adverse childhood experiences
- increased risk of substance dependence, poor mental health and early mortality Limited access to timely, appropriate services
Potential impacts for women and children
- economic insecurity and exclusion can increase financial strain on households
- accumulated trauma and stress may contribute to relationship conflict, instability, or intergenerational transmission of adversity to children
This framework is included to illustrate how masculinity interacts with inequality to shape health outcomes. It helps explain why:
- some men avoid help until crisis
- some men experience disproportionate harm from structural disadvantage
- one-size-fits-all approaches to men's health fail to reach those most at risk
Positive masculinities
While Connell’s framework helps explain how certain dominant forms of masculinity can generate risk and inequality, masculinity itself is not inherently harmful. Many traditionally masculine traits: loyalty, courage, responsibility, and pride in providing for others, can be protective and health-promoting when expressed in flexible and relational ways.
The aim of this report is to examine how masculinities can become harmful when combined with deprivation, trauma and structural change, and to promote healthier expressions of masculinity that support men, women and children alike.
Local expressions of masculinity
The Big Question explored local male experiences through in-depth, qualitative methods (Ashworth, E. et al, 2026). The industrial heritage and relatively isolated geography of West Cumbria have shaped a form of masculinity centred on hard work, close loyal workforces, and resilience. These strengths are sources of pride. However, when work becomes unstable, the same norms can produce silence, shame, or withdrawal. Men may avoid asking for help because it feels incompatible with family and cultural norms.
These socially learned norms can become health-harming when combined with poverty, trauma, grief, discrimination or limited opportunities. They help explain why men sometimes present late to services, respond to distress through anger, or turn to substances as coping mechanisms.
Inequalities: why some men are affected more than others
Inequalities: why some men are affected more than othersThe poorer health outcomes observed among men in Cumberland do not affect all men equally. Their experience depends on intersecting factors such as socioeconomic situation, place, ethnicity, disability and sexuality, which can generate cumulative disadvantage.
Boys and men who have grown up in care, live with disability, are neurodivergent, identify as LGBTQ+, or come from ethnic minority backgrounds often encounter additional barriers in education, employment, relationships and access to support. These experiences influence not only opportunities, but also whether men feel safe in expressing their identity, asking for help, or being vulnerable.
Gender norms do not affect all men in the same way. Some men socially benefit from dominant expectations of masculinity, while others find themselves constrained or harmed by them. Men who face social or economic disadvantage often experience the sharpest consequences, as expectations of self-reliance and toughness meet with limited resources, discrimination or trauma. These patterns reflect structural conditions rather than personal failure.
Place and employment
Despite employment data that appears consistent with national averages, West Cumbrian communities face long term challenges due to deindustrialisation of coal and steel production. Recent generations have experienced the effects of unemployment, abrupt changes in work identity. The local economy remains dependent on major employers like Sellafield, which offers well-paid jobs but create economic disparity. Masculine norms shaped around traditionally male roles and breadwinning can be challenging when employment is unstable or income is disparate. This is further explored in Chapter 4: Work, place and identity in adult men’s lives.
Adversity and grief
Individuals in communities with unstable work, low income, or limited opportunities often carry high cumulative grief loads, multiple bereavements, sudden losses, or traumatic events. Without the tools to express vulnerability or seek support, grief can become internalised and have long lasting psychological and/or physical impacts. The Big Question report highlighted grief as a major factor in suicide in Cumberland (Ashworth, E. et al, 2026).
Approach and frameworks
This report draws on several established public health perspectives to guide the analysis.
Life course approach
Health inequalities accumulate across time. Early childhood experiences, school environments, work pathways, relationships and community settings all shape men’s wellbeing in adulthood.
Determinants of health framework
The report considers how wider systems, such as housing, employment, social security, education, justice, and service design influence health. These structural determinants explain why individuals facing similar stresses have different outcomes.
Diderichsen’s inequalities framework
We employ Diderichsen’s framework on how inequalities emerge through differential exposure, vulnerability, consequences, and responses.
Evidence and engagement
This report was informed by engagement with a wide range of local practitioners, service leads and community organisations working with men, boys and families across Cumberland. Contributors included representatives from Cumberland Council, Cumbria Constabulary, community and voluntary organisations and sports and wellbeing organisations.
A survey was undertaken to capture professional insight into the needs of boys and young men in Cumberland. The survey was completed by 53 practitioners working across education, youth justice, family support, wellbeing and voluntary sector services. The survey captured practitioner perspectives on needs, barriers to engagement and effective approaches. The survey does not represent the views of boys and young men themselves. Findings are used throughout this report to contextualise and corroborate population-level data.