Substance misuse rates
Substance misuse ratesSubstance use is a significant public health concern in Cumberland, contributing to mortality, hospital admissions, crime and unmet support needs. In 2022 to 2024 there were 164 drug-related deaths in Cumberland, an age-standardised morality rate of 21.9 per 100,000 which is around double the national average. Cumberland had the third highest rate of local authorities nationally, with only Blackpool and Middlesborough having higher. Drug related deaths are around double in men compared to women, at 27.6 (7th highest) and 6.9 (14th highest) per 100,000 respectively, and are rising in recent years in both men and women (Figure 16) (Sources: ONS, 2024 and Cumberland statistical summary, 2025).
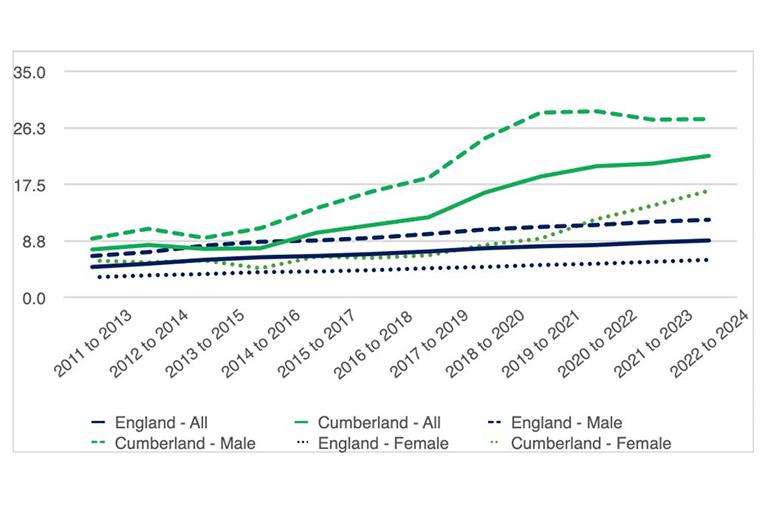
Figure 16: Drug related deaths (drug poisoning & misuse) all persons; age-standardised rate per 100,000).
Local assessment data for Cumbria indicate that there were approximately 2,400 individuals using opiates and crack, with opiate prevalence higher than regional and national averages, and around 5,594 adults estimated to be dependent on alcohol at similar rates to England overall.
In 2024 to 2025 there were 1,940 people in treatment for drug and alcohol use (source: NDTMS), 1290 (66.5%) of whom were male, 1145 (59.0%) in the 30 to 49 year age group. People with opiate dependence formed the largest treatment group (875 out of 1940, 45.1%) with the next largest treatment group being people with alcohol misuse (685 out of1940, 35.3%).
Co-occurring mental health needs are common among those entering treatment, while unmet need for treatment among dependent people persists at similar or higher levels than national benchmarks. These patterns occur alongside rising levels of drug-related crime and a growing proportion of treatment clients who are parents, underlining both the personal and social impact of substance use in the area.
Regarding children and young people, in 2023 the youth substance team received around 100 referrals for young people across both Cumberland and Westmorland and Furness. Most of these referrals were young men, with over half of referrals for drug use and around a third for alcohol use. In 2023 to 2024, there was a rate of 44.7 per 100,000 alcohol specific admissions for under-18s in Cumberland, around double the national rate and the highest rate in the Northwest of England (source: Fingertips).
National data 2023 to 2024 collated by the Office for Health Improvement & Disparities found that 21% of people started treatment in substance services had no home of their own, higher in people starting treatment for opiate problems. Almost three quarters of adults had a mental health need. Table 2 shows the national breakdown by sex of adults in contact with drug and alcohol treatment services. The age group with the highest number of people in contact is 40 to 44 years, at 53,747 individuals.
Table 2: Adults in contact with drug and alcohol treatment services between 1 April 2023 and 31 March 2024, England, by sex
| Substance group | Men | Women | Total |
|---|---|---|---|
| Opiate | 100,359 (72.7%) | 37,606 (27.3%) | 137,965 (44%) |
| Non-opiate only | 24,982 (68.4%) | 11,545 (31.6%) | 36,527 (12%) |
| Non-opiate and alcohol | 30,101 (71.3%) | 12,097 (28.7%) | 42,198 (14%) |
| Alcohol only | 56,429 (59.9%) | 37,744 (40.1%) | 94,173 (30%) |
| Total | 211,871 (68.2%) | 98,992 (31.8%) | 310,863 (100%) |
Cumberland is experiencing a crisis in drug related deaths in men and women, at 27.5 and 14.2 deaths per 100,000 population respectively. The rates of deaths have tripled for men and nearly tripled for women over the last ten years.
Safer Drug Consumption Facilities (SDCFs) are a relatively novel intervention: settings where people can consume drugs procured elsewhere while in the presence of health care professionals to reduce and respond to overdoses and offer access to healthcare and social services. Globally, many countries including Scotland have introduced SDCFs. Evaluation of existing SDCFs found they were cost-effective, reduced drug related deaths and injecting harms, associate with increased uptake of addiction care, reduced publicly discarded syringes around the facilities and can provide links to housing and mental health services. Despite the evidence in favour of SDCFs, the Misuse of Drugs Act prohibits the legal operation of SDCFs, and the UK parliament has announced their intention to keep this legislation in place, even if Scottish pilot evaluations demonstrate benefit, precluding the opening of SDCFs in England. In the face of high and up-trending drug related deaths and harms, it is important that due consideration is given to novel, potentially revolutionary drug treatment service models such as SDCFs, and that local authorities most impacted by drug related deaths advocate for these approaches.
Interpretation
While cardiovascular and respiratory disease remain important contributors to mortality among men in Cumberland, it is deaths from external causes, particularly suicide, drug poisoning and injury, that most sharply contribute to differences in men’s outcomes from both women locally and men nationally. These deaths tend to occur earlier in the life course, disproportionately affecting men of working age, and therefore contribute heavily to the gap in life expectancy. Perspectives from local practitioners and professions regarding the root causes of these patterns are explored in Box 1.
Box 1: Local professional and practitioner perspectives regarding the underlying factors in Cumberland leading to high rate of deaths due to ‘external causes’ (suicide, poisoning and injury).
Practitioners working with men and boys consistently described these deaths not as isolated events, but as the culmination of cumulative distress: unresolved trauma, economic insecurity, relationship breakdown and delayed engagement with support. This aligns with professional survey findings, where emotional suppression, trauma and low aspiration were among the most commonly observed challenges, and where the majority of practitioners reported that boys and young men often or almost always hold back from seeking help. These patterns raise the need to explore when these inequalities begin, if they can be prevented earlier and how this prevention might take shape.
Deaths of despair
The combined mortality arising from suicide, drug poisoning and alcohol-related causes is often described as “deaths of despair” (DoD). The term was originally used by economists Anne Case and Angus Deaton to describe rising mortality in the United States, particularly among White men without higher education, linked to long-term economic and social dislocation (Case & Deaton, 2022).
Subsequent research in England, including analysis by the University of Manchester, has shown a similar pattern, with deaths of despair disproportionately concentrated in the North of England and in coastal areas. This research characterises deaths of despair as an “avoidable human cost of inequitable resource deprivation” (Camacho et al., 2024). Key factors associations with DoD were living in the North, unemployment, White British ethnicity, living alone, economic inactivity, employment in elementary occupations, and living in urban areas (Camacho et al., 2024).
Many communities in Cumberland experience a clustering of these risk factors. Rising mortality due to suicide, drug-related deaths and alcohol-related harm locally reflects a pattern consistent with deaths of despair, highlighting the cumulative impact of economic insecurity, social isolation and limited access to early support. This framing reinforces the need to address upstream determinants and underlying causes of cycles of deprivation.