Conclusion and recommendations
Conclusion and recommendationsThrough this report, we aim to have demonstrated the need for a gender-focused call to action to improve health and wellbeing for the whole population of Cumberland. We have set out where health and wellbeing outcomes are poorer in men and characterised the wider determinants of these. We have examined the mechanisms of male identity formation through the life course and discussed how these identities interplay with social, economic and cultural factors to result in the picture we see today.
Crucially, we recognise that Cumberland is a changing landscape. There is growing public conversation around men’s mental health, reflected in the rapid expansion and high utilisation of voluntary and community sector provisions such as Andy’s Man Club, and increasing visibility of local grassroots discussion around masculinity and wellbeing.
With Cumberland experiencing the highest suicide rates among women of any local authority, and a clear link between these suicides and experience domestic abuse, and the third highest suicide rate overall, there is a clear need for coordinated, system-wide action that supports men’s health not in isolation, but as part of the health of families, communities and future generations.
The recommendations in this chapter are therefore framed at a system level. They focus on addressing upstream drivers of harm in ways that improve outcomes for men and reduce secondary impacts on partners, children and communities.
Taken together, these recommendations emphasise prevention, earlier engagement, cultural change and coordinated delivery across statutory, voluntary and community partners.
We are at a critical juncture. We have the opportunity to engage with the felt and expressed need of our population and respond to the clear and concerning story told by our mental health data.
Headline recommendations
Recommendation one
Apply a gender-transformative approach and challenge identity, culture and stigma drivers of health inequality.
Improving men’s health outcomes in Cumberland requires explicit attention to identity, culture and social norms, including expectations around masculinity, emotional expression and help-seeking.
Cumberland should adopt a gender-transformative approach (Box 5) that:
- challenges harmful norms without reinforcing stereotypes
- promotes diverse and positive models of masculinity
- normalises help-seeking across the life course
- applies this lens within education systems to address differential attainment and engagement patterns between boys and girls, supporting identity, belonging and aspiration from early years onwards
- ensures that work on male identity sits alongside continued commitment to preventing violence against women and girls, safeguarding children and addressing abuse
- integrates public-facing initiatives and peer-led activity with accessible service pathways
Recommendation two
Build a prevention-first, place-based system that aligns with how men engage.
Cumberland should move towards a prevention-first, place-based system of support that enables boys and men to access help early, informally and without stigma. This includes developing and expanding existing accessible wellbeing hubs or community entry points in key towns.
This requires access to support that is available through multiple entry points, including community venues, wellbeing hubs, and activity-based offers, with capacity to reach rural and coastal communities.
A prevention-first front door should prioritise:
- early engagement before crisis
- flexible access routes
- continuity of contact
- clear pathways into specialist support when risk escalates
- embed a coordinated multi-agency postvention approach following suspected suicide, including trauma-informed support for families, schools, workplaces and primary care
- recognise community and voluntary sector provision as a core part of the system, acting as trusted bridges
Recommendation three
Make men’s mental wellbeing a community-based conversation and shared responsibility.
Cumberland should treat men’s mental wellbeing as a place-based, community responsibility. Evidence from The Big Question and professional feedback shows that stigma, silence and lack of visible permission to talk remain major barriers to help-seeking, particularly in rural and close-knit communities. Community-led approaches can reduce these barriers and enable earlier support.
Cumberland should adopt a community asset-based approach to:
- fund and convene place-based men’s mental wellbeing action groups in priority areas to co-produce local priorities, shape service design and expansion
- bring together residents with lived experience, community and voluntary organisations, statutory partners and named system leads
- support locally designed public campaigns to normalise help-seeking and challenge harmful norms
This approach requires sustained investment but offers the opportunity to align services with lived experience, reduce stigma at scale and improve early engagement. Making men’s mental wellbeing a visible, shared community concern reinforces cultural change, strengthens prevention and supports more effective use of services over time.
Box 5: The Interagency Gender Working Group Gender-transformative approach
Taking a Gender-Transformative Approach
Gender-transformative approaches aim to address the structural and social root
causes of gender inequality and thereby promote more equitable outcomes across
populations. In the context of men’s health, this means examining how gender norms
and expectations shape behaviour, identity, help-seeking and exposure to risk.
The Inter-agency Working Group (IGWG) defines a gender-transformative approach as:
A transformative approach promotes gender equality by:
Fostering critical examination of inequalities and gender roles, norms and dynamics
Recognizing and strengthening positive norms that support equality and an enabling environment
Promoting the relative position of women, girls and marginalized groups
And transforming the underlying social structures, policies, systems and broadly held social norms that perpetuate and legitimize gender inequalities
Gender-transformative approaches have been adopted globally, including MenEngage, UNICEF. and Victoria Health (VicHealth), which has applied the approach specifically to masculinities and health promotion to produce Masculinities and Health: a framework for challenging masculine gender stereotypes in health promotion.
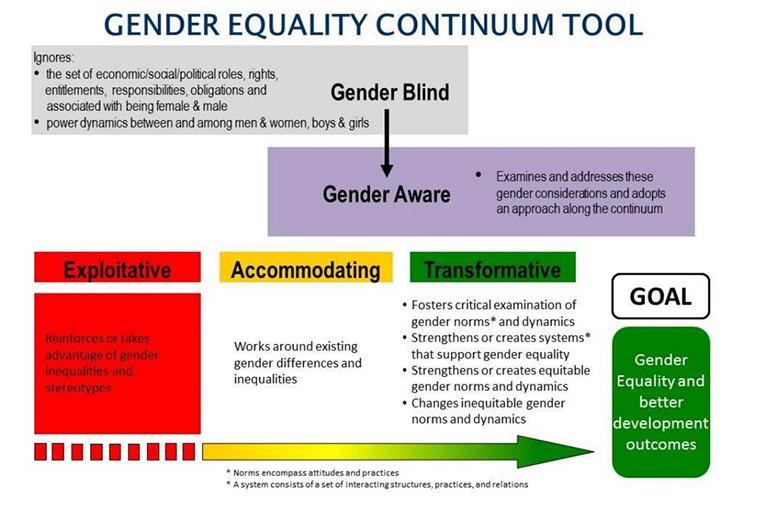
The gender integration continuum (IGWG) provides a framework for assessing whether programmes reinforce, ignore or actively transform gender norms (Source: IGWG)
In Cumberland, applying a gender transformative lens to men's health means:
Challenging restrictive norms around masculinity in both men and women, including expectations of stoicism, self-reliance and economic provision.
Recognising that gender roles are socially constructed and influence boys’ educational engagement, men’s work identities and patterns of emotional expression across the life course.
Promoting diverse and positive masculinities that value emotional literacy, caregiving, respect and community contribution.
Addressing the structural drivers of inequality, including differential attainment, occupational segregation and economic exclusion, that shape men’s health outcomes.
Ensuring that work on men’s health strengthens, rather than competes with, efforts to prevent violence against women and girls and safeguard children.
Recognising that gender is relational, and that improving men’s health requires attention to how power, status and inequality operate between women and men and among men.
Recommendations by sector and function
Recommendations by sector and functionCumberland Council
Continue the shift towards prevention, encouraging early help and reducing stigma for boys and men, prioritising life stages and groups at highest risk (including adolescence, early adulthood, working-age men and those affected by unemployment or isolation).
Embed postvention as a core prevention function, ensuring timely, trauma-informed support for individuals, families, schools, workplaces and communities affected by suicide.
Agree a concise set of important shared outcomes and indicators for boys’ and men’s wellbeing, including access, waiting times, continuity, postvention reach and inequalities by place.
Embed proportionate evaluation within new and existing initiatives, enabling learning, adaptation and scaling of what works.
Report progress publicly, ensuring transparency and accountability to communities
Strengthen early, relational support within schools, particularly for boys at risk of exclusion or persistent absence, with a focus on understanding behaviour, supporting neurodiversity and maintaining engagement in education.
NHS health and mental health services
Develop low-threshold, face-to-face access points (e.g. walk-in or drop-in mental health hubs) in key towns.
Maintain in-person routes alongside digital offers.
Simplify and increase flexibility of referral pathways, enabling referrals from GPs, schools, employers, VCSE organisations and families, and reducing repeated re-assessment or “bouncing” between services.
Strengthen crisis response and follow-up, ensuring empathic first contact, continuity after crisis and proactive re-engagement.
Improve neurodiversity pathways for all genders and ages, including workforce capacity, earlier identification and practical support for individuals and families across the life course.
Improving access to timely assessment and family support, strengthening links between schools and mental health services.
Supporting the voluntary and community sector
Formally support and connect peer-led and community-based approaches, recognising their role as entry points into the wider system rather than standalone solutions.
Strengthen coordination across VCSE providers, including shared referral routes, and clearer links to statutory services
Use visible, stigma-breaking community activity (e.g. public conversations, peer spaces, awareness events) to normalise help-seeking and reduce isolation.
Train trusted community figures to talk about mental health (e.g. barbers, sports leaders, employers, e.g. funding BarberTalk training programmes).
Encourage and support community and voluntary sectors to access additional funding opportunities.
Education and schools
Prioritise early, support for boys at risk of exclusion.
Reduce reliance on permanent exclusions by strengthening in-school support, early help links and family engagement.
Embed emotional literacy and help-seeking education within the curriculum, delivered in age-appropriate, gender-sensitive ways.
Actively raise aspiration and widen horizons, including exposure to diverse career pathway, and positive male role models from a range of backgrounds.
Employment and workplaces
Employers should recognise their workplaces as key prevention settings, equipping managers and trusted staff to identify distress, provide early support and signpost effectively.
Employers should support encourage diverse access into employment, including men into health, education, and administration.
Workplaces should lead the way in recognising and supporting men to be joint-primary caregiver.
Justice system (including prison and probation)
Strengthen the health–justice interface, ensuring continuity of mental health, substance misuse and neurodiversity support during custody, probation and transition back into the community.
Integrate family-focused and relational support into justice pathways to reduce intergenerational harm and repeat cycles of disadvantage.
Conclusion
ConclusionThis report has examined men’s health and wellbeing in Cumberland across the life course, showing a pattern of consistently poorer outcomes in some areas, high exposure to risk and later engagement with support. These outcomes are shaped by place, deprivation, rurality, employment patterns, neurodiversity and life transitions, rather than by individual behaviour alone.
A central finding of this report is that many boys and men delay seeking help because support feels inaccessible, stigmatising or poorly aligned with how distress is experienced and expressed. Services that rely on crisis thresholds, short-term interventions or verbal disclosure often engage men too late. In contrast, relational, activity-based and community-embedded approaches support earlier engagement and more sustained connection.
Cumberland has strong foundations to build on, including committed partners, active communities and examples of effective practice. However, improving outcomes will require a shift from fragmented provision towards a coordinated, prevention-first system that addresses identity, culture and aspiration, strengthens education pathways, and aligns services with lived experience.
The recommendations in this report set out a practical framework for action. By acting on this evidence, Cumberland has an opportunity to improve outcomes for boys and men while reducing avoidable harm to families and communities, and to build a healthier, more resilient future.