Health outcomes are shaped by wider determinants of health (Figure 1): the social norms that we inherit, the socioeconomic conditions we live in, the relationships and expectations that surround us and the cultural norms that shape communities over generations. These factors interact with the local infrastructure, service accessibility, influencing what kinds of help they seek, what kind of actions they take and what sort of opportunities and futures feel visible and possible.
Gendered expectations describe the societal norms and stereotypes around how individuals should act, present and behave based on their sex. Commonly cited and investigated domains on gendered stereotypes include personality traits, role behaviours, occupational and emotional.
Frequently, men’s health is described through a language of personal actions or failing of action; men ‘don’t talk’ or ‘won’t seek help’ or are ‘risk takers’. Similarly to expressions such as ‘man-up’ or ‘grow some balls’, the language used to describe masculine health seems to assume that poor health is driven by personal failings and individual actions. While individual actions matter, this framing does not sufficiently recognise the influence of the social norms of what it means, or does not mean, to be a man, and how this shapes our communities and individuals. In Cumberland, these norms are shaped by a history of industrial work, de-industrialisation, tight-knit communities and a longstanding local culture towards stoicism and emotional self-reliance.
This chapter provides the conceptual grounding for understand the patterns of men’s health outcomes seen across Cumberland. It aims to situate male health inequalities in sociological context, to explore how masculinities develop and result in differential health outcomes.

Figure 1: The building blocks to health by the Health Foundation
How men's, women's and children's health interconnect
The phrase ‘health is not a zero-sum game’ is often used in relation to health. This phrase addresses the concept that one person’s health gain is another person’s health loss. ‘Positive sum’, are health investments that have wider impacts beyond the primary aim, such as improved physical health leading to improved economic productivity or social connection, simultaneously benefiting others in immediate and wider circles.
Men and women’s health are interdependent. Individual, partnership, societal and systemic interactions between genders influence physical, mental and social health.
Poor male health, whether through chronic illness, addiction, or mental ill-health, has consequences for women and children. Women may carry increased caring responsibilities, face financial strain, or encounter emotional and physical risks within relationships. Children exposed to instability, conflict or trauma may have poorer health and emotional wellbeing outcomes, which in turn can shape the outcomes of the next generation of men.
Parental wellbeing directly affects children’s emotional security, educational attainment and health development, influencing how children grow and behave. Household stressors such as poverty, grief, insecure work and poor-quality housing are experienced collectively.
From a sociological perspective, gender operates as a social system: a set of rules, expectations and practices that shape how people behave and how society responds to them. We adopt a gender-relational lens: the health of one group cannot be understood or improved without analysing gender differences, dynamics and social norms, allowing us to identify systematic drivers and design targeted solutions.
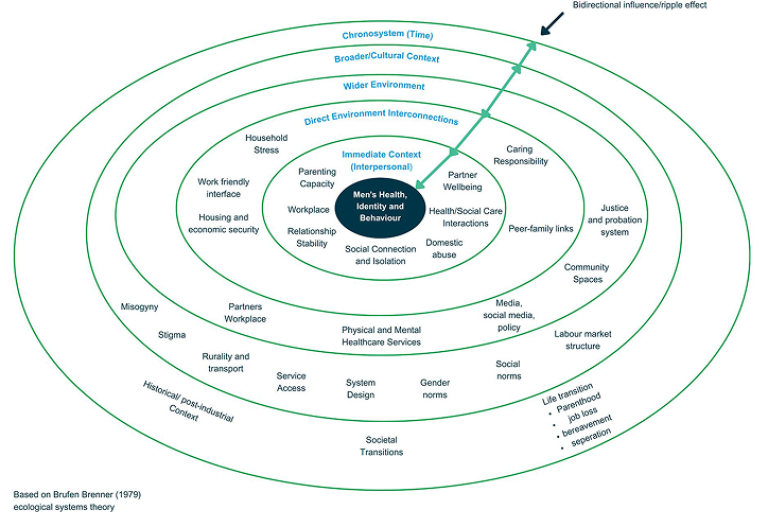
Figure 2: The bi-directional interactions between men’s health and identity, and relationships, environment and cultural. Adapted) ecological systems theory (Bronfenbrenner, 1979).