For many men in Cumberland, psychological distress is closely linked to experiences of redundancy, insecure employment, declining physical capacity or perceived failure to meet provider roles (Ashworth, E. et al, 2026). Contact with the justice system factor is also associated with poor mental health, with half of the boys and men in contact with the justice system reporting anxiety or depression, compared with 15% of the general population. Cultural norms that value stoicism and “getting on with it” can discourage early disclosure, leading men to internalise distress and delay seeking support. As a result, mental health difficulties frequently come to attention only once they have escalated, often alongside physical illness, financial strain or crisis events, with consequences that extend beyond individual men to families, workplaces and communities.
Available data on mental health and wellbeing is generally scarce and not available split by sex. Where data is available, the ratio of higher suicide rates in men compared with women does not tend to correlate with diagnosis of mental health conditions. NHS England population survey data conducted every seven years since 1993 show that women have a higher prevalence of diagnosed common mental health conditions than men across all age groups at all time points, including anxiety disorders, depression and phobias.
A local survey in the Cumberland, conducted by The Big Question study (explored further in the next section) found that a higher proportion of men reported thoughts of self-harm compared with women (52% vs 47%), however women were slightly more likely to have previously ever self-harmed (28% vs 25%), and slightly more likely to seek help (57% vs 51%) (Ashworth, E. et al, 2026). Participants reported varying quality of help received; while some were supported by healthcare organisations, there was report of private therapy, third-sector organisations (e.g. Andy’s Man Club and Samaritans) and organisations outside of Cumberland.
Key challenges in seeking help were varied and somewhat echoed those in surveyed professionals supporting children and young people. Some Big Question respondents reported self-reliance and management, stigma, previous negative experiences, difficulty in asking for help, accessibility, lack of long term support for men and feeling they had to reach crisis point before being eligible for support.
These findings echo wider knowledge that men are less likely to report symptoms or engage with services at an early stage, and are more likely to present later, with more severe or complex manifestations of distress. This helps explain why men in Cumberland experience disproportionate rates of mental health-related economic inactivity, substance use and suicide, despite lower diagnosed prevalence of common mental health conditions.
Debt and gambling harms
Gambling is widely known to be a harmful commodity, impacting on psychological and physical health. While overall gambling levels are highest in people with better psychological health and life satisfaction, at-risk and problem gambling prevalence is higher in those with poor health, low life satisfaction and wellbeing (source: NHS England). Being male and having poor mental health are strong predictors of at-risk gambling.
In understanding patterns of gambling, one challenge is the reliability of data. Much of what is available, and quoted below, comes from GambleAware; this is an organisation funded primarily by voluntary donations from the UK gambling industry and has previously faced scrutiny over conflicts of interest regarding ties to the industry and lack of independence concerns, including in a case raised by the Good Law Project which was later closed by the Charity Commission. The data that follow should therefore be seen in this context.
In 2020 data collated by GambleAware, around 7% of the population of Great Britain were negatively affected by someone else’s gambling. In 2020, Of the 7%, affected others were more likely to be a women, 25% were a spouse or partner, 21% were a mother or father, while 9% were a son or daughter. Impacts were felt most severely by partners, parents or children of problem gamblers.
In further data collected by GambleAware, through the Annual GB Treatment and Support Survey 2024, Cumberland appears to have gambling problems below the national average. It is important to note the limitations of the Problem Gambling Severity Index (PGSI), the screening tool used to assess problem gambling. The tool assesses for presence of harms at that moment only, not severity of harms, wider impacts or ongoing to harms to people who have previously had gambling. However, this still generated an estimated fiscal cost of £5,542,704 of harms associated with gambling, predominantly though welfare costs and hospital inpatient stays.
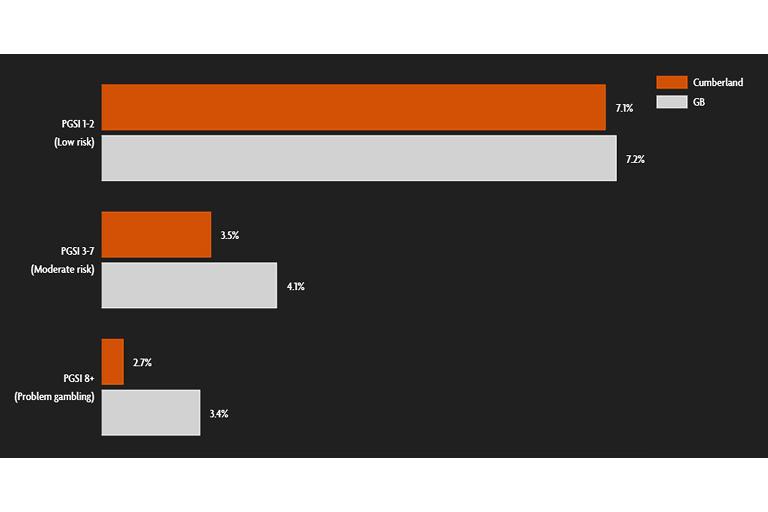
Figure 14: Prevalence of gambling problems, Cumberland and Great Britain, 2024.
Direct harms to gamblers were financial harms, relationship harms, mental and physical harms (those with a gambling disorder have an increased risk of all cause mortality), employment and education harms, criminal harms and cultural harm (source: OHID, PHE). These are echoed in harms felt by those impacted by harm, with 75% reporting feelings of anger, anxiety, depression, sadness, or distress and 60% reporting negative financial impacts (source: GambleAware).
Men and women demonstrate differing patterns of gambling behaviour and associated harms. Research consistently finds that men are more likely to engage in higher-risk, competitive and rapid-cycle forms of gambling such as sports betting, poker, online betting and casino gambling, whereas women are more likely to participate in chance-based formats such as gambling machines (Baggio et al., 2018). Males gamble proportionately more than females, except regarding scratch cards. Harmful gambling among men has been more strongly associated with sports betting and substance use, whereas among women it appears less associated with substance-use networks (Baggio et al., 2018).
The structure of gambling activities also differs in ways that may influence harm. High-intensity formats such as online sports betting and casino games are characterised by rapid cycles of staking and reward, and greater opportunities for escalation and solitary play, whereas other formats are more socially embedded. Recent research indicates that for both men and women, gambling motivated by coping is strongly associated with severity of harm, with maladaptive emotion regulation emerging the key predictor (Theodorou et al., 2025).
The National Men’s health strategy highlights gambling as key concern in men’s health. Men were highlighted as more likely to experience gambling rating harms, to gamble online and engage in online gambling, increasing exposure to gambling-like content. A new national gambling tax law was announced in the 2025 budget and provides protected funding for gambling harms prevention (30% of levy funding), treatment (50% of levy funding), and research (20% of levy funding). The Government has committed to developing a coordinated approach to gambling prevention, including a new voluntary sector grant, delivering a research programme and increasing treatment and support services. It is imperative that Cumberland advocates for shared receipt of these resources and that statutory organisations support voluntary sectors in doing so.
Suicide rates
Across the UK, suicide and injury or poisoning of undetermined intent is the leading cause of death for both males and females aged 20 to 34 years. Men were more than three times as likely to die by suicide compared with women in this age group. Since 2001, the leading cause of death in men aged 35 to 49 years has changed from ischaemic heart disease to suicide in 2011-2015 and accidental poisoning more recently (source: ONS).
In 2022 to 2024, there were 137 suicides in men and women in Cumberland, the third highest out of 153 upper tier local authorities in England and a rate of 19.4 per 100,000 population (source: ONS). Suicides rates in Cumberland are increasing, and at a higher rate compared with England.
In 2022 to 2024, men in Cumberland had the 7th highest rate of suicide deaths nationally. Of the 137 suicide deaths in Cumberland, 98 were in men. This is a rate of 28.2 per 100,000, significantly above the national rate of 16.8. In the same period, women in Cumberland had the highest rate of suicide related deaths, with a rate of 11.2 per 100,000 compared to 5.5 per 100,000 nationally. This is further explored in Chapter 4: Work, place and identity in adult men’s lives.
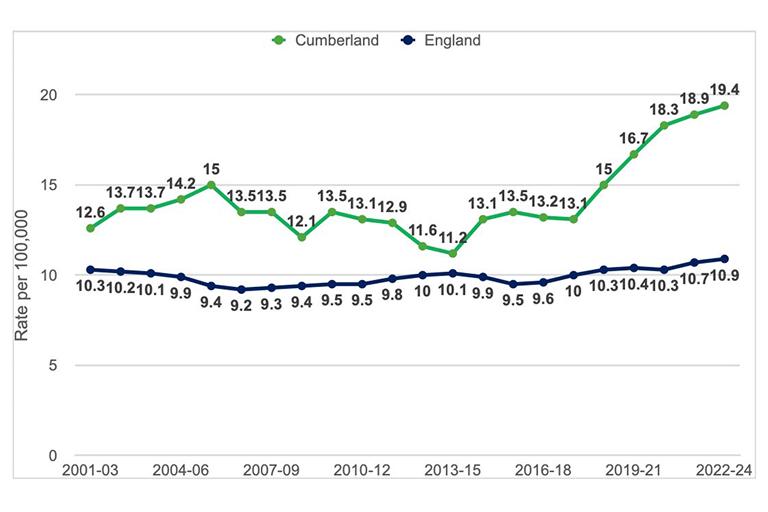
Figure 15: Suicides: Cumberland and England; 2001 to 2024 Age-standardised Rates per 100,000 population (Source: ONS)
Suicide: the big question
Suicide rates in Cumberland show a persistently high burden, particularly among men. This fact prompted The Big Question, a mixed-methods study commissioned by Cumberland Council and undertaken by Liverpool John Moores University, to explore why suicide risk remains high and how it is experienced locally (Ashworth, E. et al, 2026).
Men and women were similarly likely to report suicidal thoughts (57% of men compared with 55% of women), and men were slightly more likely to report having received support. Of the 40 men who reported a previous suicide attempt, 27 (67.5%) reported receiving support after (although only 30 gave responses). Of 99 reporting suicide attempts, 52 received support (52.5%), with 94 out of 99 responding to this question. These findings suggest that high male suicide mortality in Cumberland is not by total disengagement from services, but by more complex factors. However, it may also be that those responding to the survey are a selection of people more likely to engage with health services than the general population.
Respondents were asked to comment on mental health challenges and contributing factors to the high suicide rates in Cumberland. Responses included mental health conditions, chronic pain and other long-term illness, neurodivergence (often diagnosed late), intergenerational trauma and adverse childhood experiences. Drugs and alcohol were described as coping mechanisms, and the long-term impact of suicide bereavement was prominent, with over half of respondents reporting being affected by the death of someone who died by suicide. Of the 781 respondents, 52% reported havening been bereaved or affected by the death of someone who died by suicide. This was lower in men than women (44.6% vs 55.2%). Common relationships were friend, family and work colleague, with many participants citing knowing more than one person who died by suicide.
Acute triggers reported to precede crisis included relationship breakdown, abusive relationships, interpersonal conflict and bullying. Environmental and socioeconomic stressors were also prominent, including isolation, rurality and transport barriers, financial strain, seasonal factors (poor winter weather), limited recreational opportunities and a labour market shaped by a small number of dominant employers. Some respondents highlighted access to firearms within agricultural settings as a specific risk factor, while social media was described as increasing isolation and undermining communication.
Attitudes and assumptions are known to shape help-seeking. Suicide was perceived as taboo for many, with suicidal thoughts often minimised or normalised. A “Cumbrian tendency” towards stoicism and emotional restraint among men was frequently cited, alongside shame and concerns about confidentiality in close-knit communities. Attitudes to mental health were reported to be shifting across generations to become less conservative and more liberal. Frustration with the availability and continuity of support was common.
Taken together, these findings reinforce and evidence that suicide in Cumberland reflects the interaction of identity-based pressures, place, constrained opportunity and delayed help-seeking. Men may articulate distress and access support at points, but remain vulnerable where help is fragmented, short-term or poorly aligned with lived realities. Addressing suicide risk therefore requires approaches that recognise identity and place as determinants of health, alongside timely, sustained and culturally aware support.
Suicide risk therefore requires approaches that recognise identity and place as determinants of health, alongside timely, sustained and culturally aware support.