The men’s health strategic vision for England, published in November 2025, highlights key foci for physical health of men, including:
- high levels of frailty in ‘young old’ populations who are sleeping homeless and 30 year earlier death compared with the general population. It is mainly men who are homeless and rough sleeping
- rates of cancer, circulatory and respiratory conditions drive much of the difference in life expectancy between the most and least deprived men nationally. Risk factors for these conditions, such as smoking and obesity, are higher in the most deprived areas of the country
- men develop cardiovascular disease around six years earlier than women
- there is a higher prevalence of type two diabetes in men
- cancer incidence and mortality is higher in men than women above the age of 60 years
- cancer incidence rates are 19% higher for men in the most deprived quintile compared with the least deprived quintile
- men carry the greatest burden of respiratory disease, particularly those who smoke, are former industrial workers and live in the most deprived communities
- two thirds of live disease is in men, linked with alcohol consumption, obesity and viral hepatitis
The strategy includes a plan, formed around meeting men where they are.
Major commitments include:
- the investment of £3 million over three years from April 2026 into community-based men’s health programmes, targeting areas at highest risk
- men's health training for healthcare professionals via new e-learning modules
- workplace health pilots in male-dominated industries through the Keep Britain Working Vanguard Programme
- enhanced lung disease support for former miners via the Respiratory Pathways Transformation Fund
- home PSA testing for prostate cancer patients from 2027 via the NHS App (subject to clinical approval)
- £200,000 trial of interventions to tackle rising cocaine and alcohol-related cardiovascular deaths
An additional major investment from national government has been the Premier League’s Together Against Suicide initiative with the Samaritans, embedding match day messages and support at stadiums. While positive, this strategy fails to recognise the lack of premier league teams in the areas with the highest suicide rates, including Cumberland, Westmorland and Furness, Blackpool, and Darlington. While the strategy is welcomed, it must be ensured that interventions do not neglect those most at risk.
In the 2022 health survey for England, men were slightly more likely to self-report good health compared with women (76% vs 74%), and less likely to report acute sickness. Women more commonly reported musculoskeletal conditions, mental, behavioural and neurodevelopmental conditions and conditions of the digestive system, while men more commonly reported heart and circulatory conditions.
Hypertension and cardiovascular health
Deaths due to circulatory causes is one of the leading causes of health inequalities both within and outwith men in Cumberland (Figure 7 and Figure 8). Men are more likely to have hypertension ‘all’ and untreated hypertension than women. Modifiable risks factors for cardiovascular disease accumulate over a lifetime (obesity from childhood, poor diet, lack of exercise, alcohol consumption, obesity), while early intervention for cardiovascular health has the potential to be highly effective, if utilised. Psychological trauma and chronic stress are increasingly being recognised as increasing risk of cardiovascular disease (Song et al., 2019).
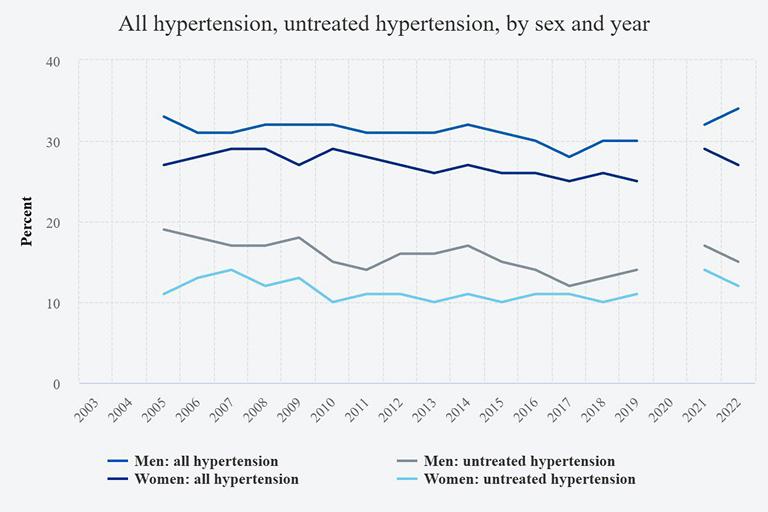
Figure 11: Prevalence of hypertension in adults in England, all and untreated, by sex and year, 2003 to 2022.
NHS Health checks are important appointments offered free to adults age 40 to 74 years, five yearly, to assess for signs of chronic conditions including cardiovascular disease. Uptake of checks in Cumberland was 27.4% in 2024 to 2025, below the national average of 37.5%. There is a stark gap in publicly available data for NHS health check uptake by gender. The last national figures on 2017 to 2018 data showed women were more likely to attend than men (44% vs 38%). Locally acquired data for 2024 to 2025 reflects this pattern, with 3,951 females attending for health checks, compared with 3,222 males.
Fingertips data indicates that men in Cumberland have higher levels of certain risk factors: smoking (three percentage points higher) and overweight and obesity (10 percentage points higher), although women have higher levels of physical inactivity (three percentage points higher).
Preventative pathways such as routine health checks rely on proactive help-seeking, yet men are less likely to engage with these services, increasing the likelihood that cardiovascular disease is first identified at either a more advanced stage, or at the point of fatal consequence. As with other health conditions, this pattern reflects not a lack of concern for health, but the interaction between masculine norms, work pressures and service design.
Prostate cancer
Other than skin cancer, prostate cancer is the most common cancer in men both nationally and in Cumberland, with risk increasing with age (Figure 12). However, lung cancer is the leading cause of cancer death nationally.
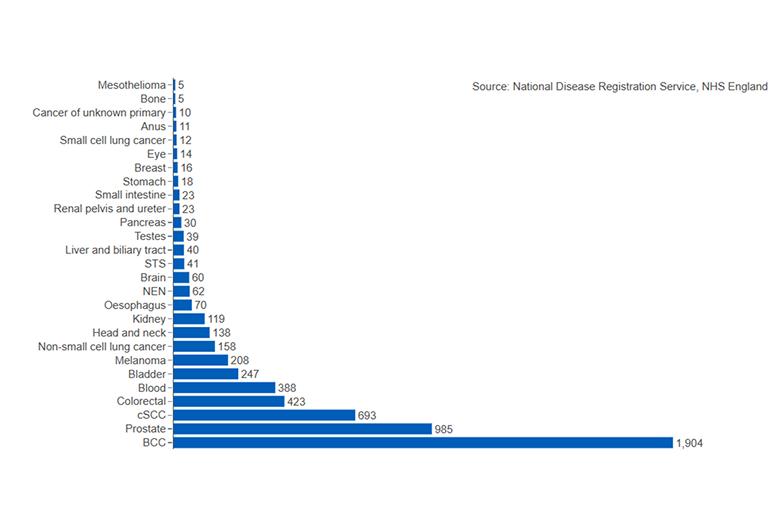
Figure 12: Number of men living with and beyond cancer in Cumberland, 2022, by cancer site. Abbreviations: Soft Tissue Sarcoma (STS), Neuroendocrine Neoplasm (NEN), Cutaneous Squamous Cell Carcinoma (cSCC), Basal Cell Carcinoma (BCC). (Source: National disease registration service)
For the 12 months ending October 2025, lower proportions of people were diagnosed with prostate cancer during the early stages, one to two, in Cumberland compared with England (53.8 vs 57.5%). The difference between local and national early stage diagnosis has been reducing since 2022 (Figure 13).
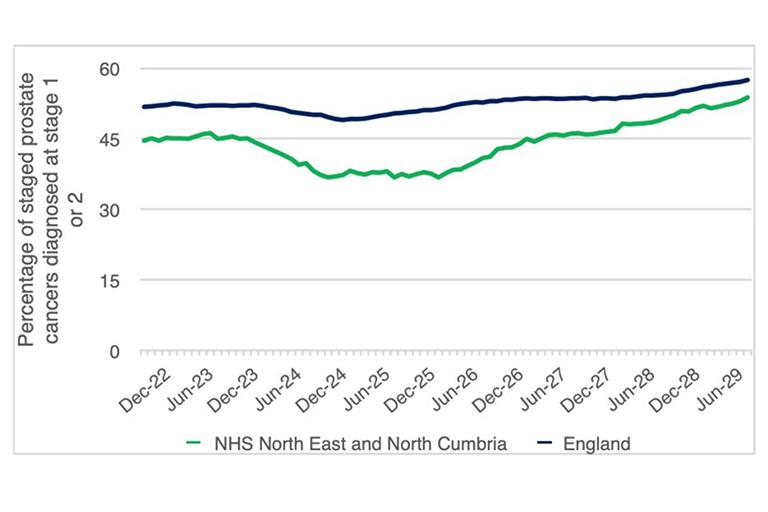
Figure 13: Prostate cancer 12 month rolling early stage at diagnosis proportion (stages 1 and 2), January 2019 to October 2025.
There is currently no national screening programme for prostate cancer. While this remains a contested decision, the conclusion of the UK National Screening Committee remains that the current available screening tests are not fully reliable at picking up cancers that actually need treatment, and some of the investigations and treatments are invasive and harmful, not balancing the need for a screening programme to do more good than harm. However, a targeted approach to screening based on risk is currently being considered.
Instead, diagnosis with prostate cancer relies on individuals presenting to medical services with symptoms such as frequent nighttime urination, weak stream of urine or difficultly passing urine.
The pattern of high proportions of later stages of diagnosis of prostate cancer in Cumberland may represent later presentation and delayed engagement with diagnostic pathways, consistent with wider evidence on men’s health-seeking behaviour locally, including lower uptake of preventative care and a higher tendency to seek help only at crisis point.